HII Weight Management Program
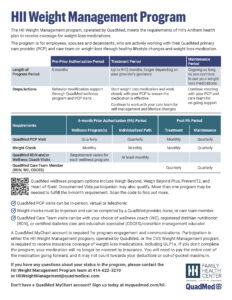
The HII Anthem medical plan requires a prior authorization for coverage of weight loss medications. One of the criteria for prior authorization includes participating in a weight management program. Your participation in the HII Weight Management Program meets the HII Anthem medical plan requirements to receive insurance coverage of weight loss medications, including GLP-1s.
Designed with your goals in mind, the HII Weight Management Program can help you manage your weight, adopt healthier eating habits, and/or increase physical activity. Your dedicated care team will offer support, motivation, and the educational tools you need to succeed at improving your overall health.
HII Weight Management Program Patient Eligibility:
- Established care and elected a QuadMed primary care provider (PCP)
- Enrolled in an HII Anthem medical plan
- HII employee or eligible dependent
- 18 years or older
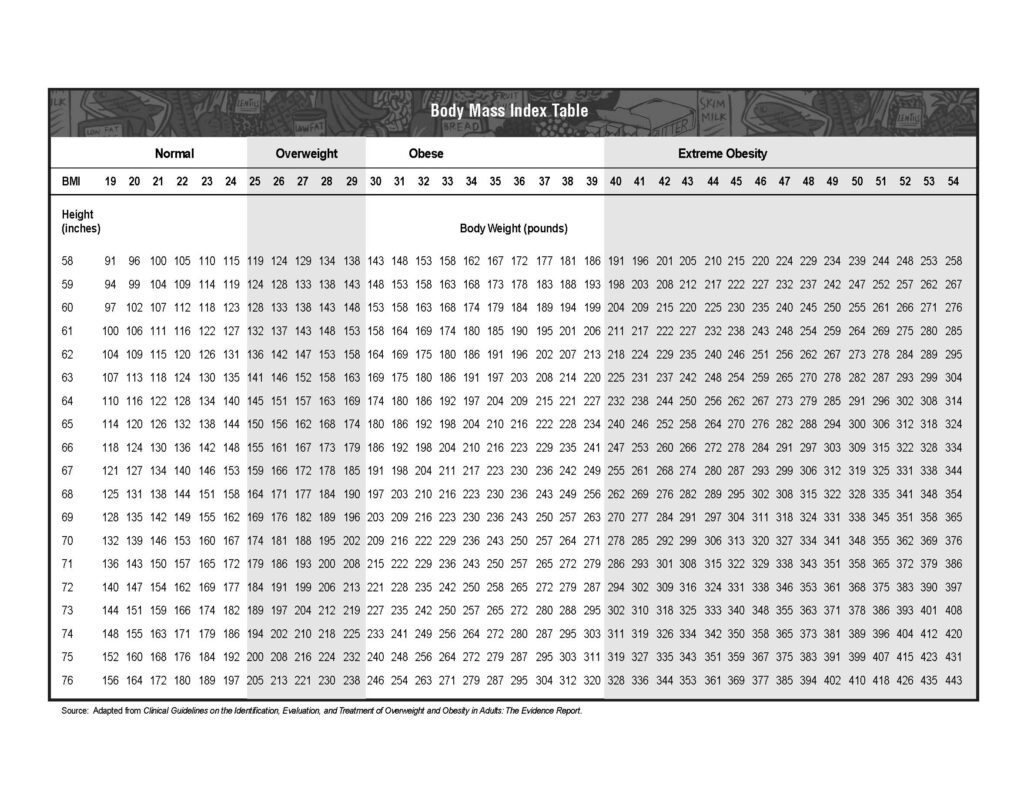
- BMI >30 or >27 + comorbidity
- MyChart activation is required once accepted to the program
If you do not have an established QuadMed PCP and still want weight loss medication coverage, you can schedule an appointment with a QuadMed provider to elect them as your PCP or participate in the CVS Weight Management Program.
If you are not enrolled in an HII Anthem medical plan, are a minor or do not meet the BMI requirements, you are not eligible for either the HII or CVS weight management programs.
This program is comprised of three periods – pre-prior authorization, treatment, and maintenance, and is at no additional cost to you. Specific criteria are required for each program period. Please refer to the patient program handout for more details.
A MyChart account is required for program engagement and communications. If you don’t complete the program, your medication will no longer be covered by insurance. You will need to pay the entire cost of the medication going forward, and it may not count towards your deductible or out-of-pocket maximum.
Requiring a patient to get prior authorization for certain medications is a common practice used by insurance companies to ensure safe and appropriate medication use.
Some medications require prior authorization, or PA, and it means that your doctor will have to provide additional information on why they are prescribing this medication for you. CVS Caremark will review this information and based on your HII health plan and determine whether the medication will be covered.
This information and process is confidential. Your medical information is not shared with HII.
Get Started

To get started, schedule a visit with your QuadMed primary care provider (PCP) by calling the HII Family Health Center in Newport News (757-327-4200) or Ingalls (228-205-7700) or online through your QuadMed MyChart account.
If you have any questions about your status in the program, please contact the HII Weight Management Program team at 414-622-3210 or HIIWeightManagement@quadmedical.com.
Don’t have a MyChart account? Sign up today!